ITUP Blog: California’s Final 2020-21 Budget
By Katie Heidorn, Garrett Hall, and Marissa Kraynak
California’s Final 2020-21 Budget
On June 29, 2020, Governor Newsom signed the Budget Act of Fiscal Year (FY) 2020 – 2021 into law following negotiations with the Legislature. The budget includes several budget savings mechanisms to address the funding shortfalls of $18 billion to $54 billion predicted by the Legislative Analyst’s Office (LAO) and the Department of Finance(DOF), respectively.
Unsurprisingly, the COVID-19 pandemic greatly influenced the state’s budget and will continue to do so over the next several months as the state received final tax returns on July 15, 2020, and potential additional federal stimulus funds. This blog summarizes the 2020-2021 Budget Act and is the third in ITUP’s Budget Blog series in addition to Five Topics to Watch in the May Revise and Key Items in the May Revise.
Here are quick links to the:
- Budget Bill (Budget Act of 2020): Senate Bill (SB) 74, Chapter 6, Statutes of 2020.
- Budget Bill Jr. (this is a supplemental budget bill, in addition to SB 74): AB 89, Chapter 7, Statutes of 2020.
- Health Trailer Bill(s)
- Human Services Trailer Bill(s)
1. Final Budget Act of 2020 Overview
2020 Budget: On January 10, the Governor’s budget predicted a $5.6 billion dollar surplus. Following the arrival of the COVID-19 pandemic, however, the May Revision and the LAO predicted a budget shortfall of $18 billion to $54.3 billion. The final budget forecasts an operating deficit of $8.7 billion in FY 2021 – 2022.
Health and Human Services: The Budget Act of 2020 includes $179.6 billion ($44.8 billion General Fund (GF) and $134.8 billion other funds) for all health and human services programs. Additionally, the Budget Act uses $450 million of the Safety Net Reserves in 2020-2021 to prevent reductions to California Work Opportunity and Responsibility to Kids (CalWORKs) program and Medi-Cal services. The Budget Act also relies on “triggers”—many programs proposed to be impacted by state budget cuts would not have their funding reduced if the federal government provides additional federal stimulus funds to the state. See Control Section 8.28 of SB 74, the Budget Act of 2020 for details on the specific impacts. While the May Revision proposed to include many health and human services programs’ funding under these trigger provisions, they were generally not included in the final budget triggers.
Public Health and COVID-19: To continue to combat COVID-19, the Budget Act includes key funding for public health. The Budget Act includes $5.9 million GF for FY 2020 – 2021 and $4.8 million GF ongoing to support the state testing laboratory staff and equipment. It also maintains the funding for infectious disease prevention and control that was scheduled for suspension January 1, 2022. In addition to state funds, more than $600 million federal funds are available to support population public health measures such as testing and contract tracing. [i]
2. COVID-19 Impacts on the Medi-Cal Program
The Medi-Cal program budget is 16 percent higher in total cost from $99.5 billion ($22.7 billion GF) in 2019-2020 to $115.4 billion ($23.6 billion GF) in FY 2020 – 2021. The increased allocation is largely due to the COVID-19 pandemic and associated effects that the crisis has had on California’s population.
Increased Medi-Cal Enrollment: As of June 2020, Medi-Cal enrollment was nearly 13 million; the Department of Health Care Services (DHCS) expects that number to increase to 14.5 million by July 2020 and proposes to dedicate $898.6 million ($319.0 million GF) in FY 2019 – 2020 and $6.9 billion ($2.4 billion GF) in FY 2020 – 2021 to it. This means that nearly 2 million people who were uninsured or lost their insurance and became uninsured will have access to full-scope Medi-Cal benefits, including primary care, specialty care, behavioral health, hospital services, dental, and pharmacy, at very low or no cost to them. Medi-Cal enrollment data is still in the process of being updated and published; you can find updated enrollment data here.
FMAP Increase of 6.2 Percent Provides Additional Federal Funding Relief: The federal Families First Coronavirus Response Act temporarily increases the Federal Medical Assistance Percentage (FMAP) by 6.2 percent. California’s base FMAP rate will increase from 50 percent to 56.2 percent, meaning that California and the federal government will share costs for Medi-Cal with California paying 43.8 percent and the federal government paying 56.2 percent of the cost instead of California paying 50 percent and the federal government paying 50 percent of the cost.[ii] The increased FMAP allows California to save $5.1 billion GF through June 30, 2021.[iii]
3. Medi-Cal Coverage Programs—Final Budget Impacts on Consumers
The Budget Act of 2020 maintains most existing Medi-Cal program eligibilities.
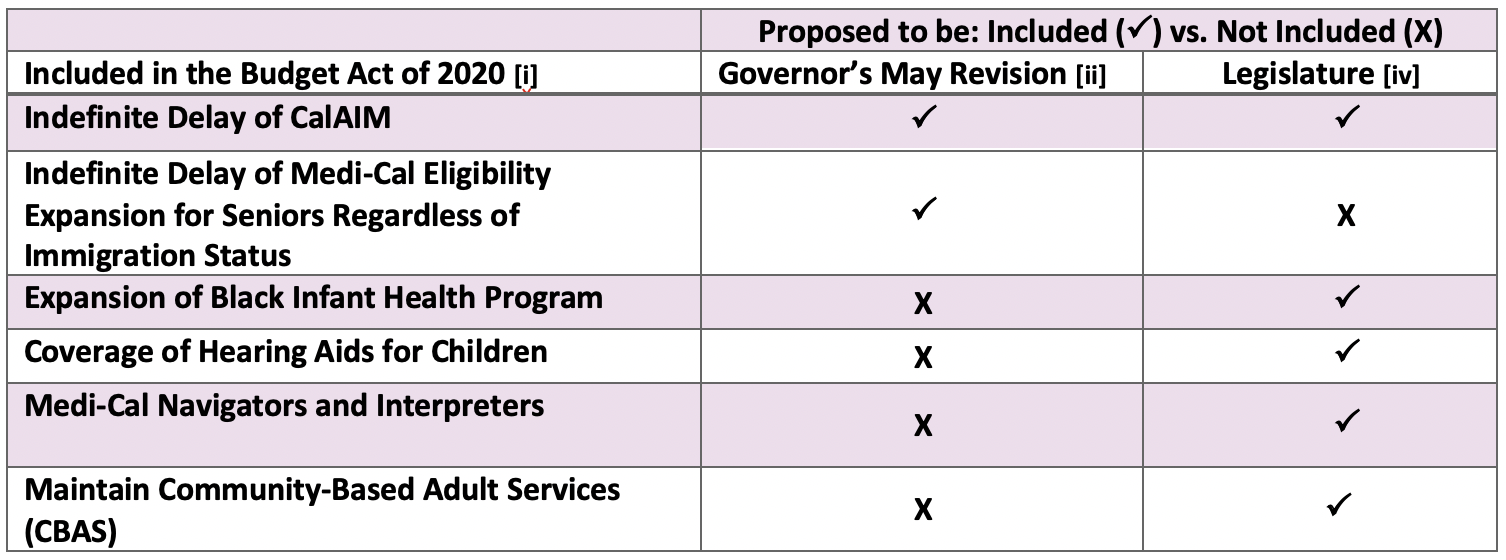
- Excluded from the 2020 – 2021 Budget Act:
-
- Expansion of Medi-Cal eligibility to seniors aged 65 and over regardless of immigration status: The Budget Act includes trailer bill language that will prioritize the expansion in the Budget Act of the next fiscal year if the DOF projects a positive ending balance in the Special Fund for Economic Uncertainties for each of the next four fiscal years. The fund balance must be more than the cost of full-scope Medi-Cal benefits to senior individuals regardless of immigration status.[iv][v]
- CalAIM: The California Advancing and Innovating Medi-Cal (CalAIM) initiative, a Medi-Cal reform program, is withdrawn, saving $695 million ($347.5 million GF) in 2020-21.[i]
- Included in the Budget Act of 2020:
- Suspended Benefit Programs: Effective December 31, 2021, Medi-Cal coverage of audiology and speech therapy, incontinence creams and washes, optician and optical lab services, podiatry, screening and brief intervention and referral for treatments related to opioids and other illicit drugs will be suspended. This framework was included in the Budget Act of 2019. [vi]
- Medi-Cal Estate Recovery: The Budget Act does not reinstate the Medi-Cal Estate Recovery policy, which pre-2016, served to recover the costs of health care services from deceased beneficiaries’ estates. The budget includes $16.9 million GF to continue the recovery policy that only recovers long-term care costs. [i]
- Home Visiting and Black Infant Health (BIH) Program: The Budget Act maintains funding for this program amounting to $65.3 million ($30.5 million GF). This California Department of Public Health-run program works to improve African-American infant and maternal health.[i] There are well-documented maternal mortality racial health disparities and the BIH program reports, “African-American mothers are four times as likely to die from pregnancy-related causes as White mothers.” [vii]
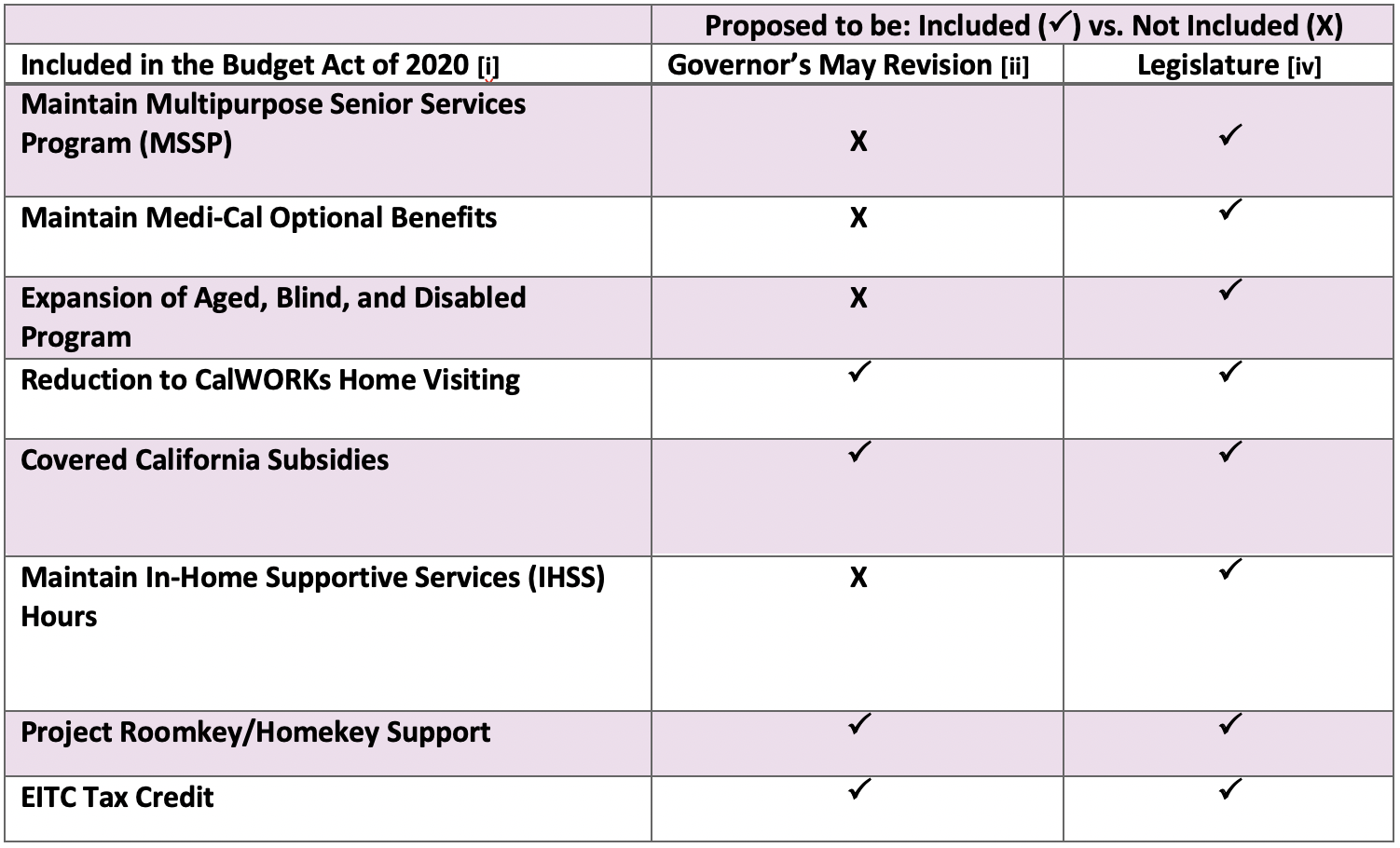
- Funding Support for Seniors: The Budget Act maintains ongoing funding for the Community-Based Adult Services (CBAS) program and Multipurpose Senior Services Program (MSSP). Both programs support California’s vulnerable seniors. CBAS is a community-based day health program serving older adults with health conditions who are at risk of needing institutional care. CBAS is expected to cost $194.4 million ($96.8 million GF) in FY 2020 – 2021 and $461.7 million ($230.7 million GF) in FY 2021 – 2022. [ii] According to the California Department of Aging, CBAS served 36,031 individuals at 257 centers statewide in FY 2019 – 2020. [viii] The MSSP program provides Home and Community-Based Services, including care management at home, using available community resources, and purchasing needed services for Medi-Cal eligible individuals who are over age 65, disabled, and residing in a county with an MSSP site to prevent or delay individuals from moving into a skilled nursing facility. [viii] MSSP is expected to cost $37.6 million ($22.2 million GF) in FY 2020 – 2021. The program serves approximately 11,370 individuals annually across 38 sites statewide. [viii]
- Hearing Aids for Children: Allocates $352,000 GF in 2020 – 2021 to establish a program to assist with the cost of hearing aids and related services for uninsured children in families with incomes up to 600 percent of the federal poverty level, effective no earlier than July 1, 2021. To administer this benefit completely, the Budget Act assumes an approximate cost of $15 million GF. [i]
- Medi-Cal Optional Benefits: Maintains ongoing funding for full adult dental services, acupuncture, optometry, nurse anesthetist services, occupational and physical therapy, pharmacist services, and Diabetes Prevention Program. [i] These benefits were initially proposed to be cut in the May Revision, contingent upon additional federal funding.
- Expansion of Medi-Cal Aged, Blind, and Disabled Program: Allocates $135.5 million ($67.7 million GF) to expand this program for qualified individuals with incomes between 123 percent and 138 percent of the federal poverty level. [i]
- Medi-Cal Navigators and Interpreters: Includes one-time $15 million GF for the Medi-Cal Health Enrollment Navigators Pilot Program and one-time $5 million GF for the Medi-Cal Interpreters Pilot Project. [i]
- In-Home and Supportive Services (IHSS) Hours: Maintains IHSS service hours, costing $357.6 million GF. The May Revision had proposed to cut the number of IHSS service hours. [i]
- CalWORKs Home Visiting Program: The Budget Act includes a one-time reduction of $30 million GF/Temporary Assistance for Needy Families (TANF). The program will continue to serve clients already enrolled in the program. [i]
- Food Banks: A one-time increase of $50 million GF for existing Emergency Food Assistance Program providers, food banks, tribes, and tribal organizations to mitigate increases in food needs among low-income and food-insecure populations. [i]
Other Consumer Impacts:
- Covered California Subsidies: Preserves the insurance subsidies for middle-income enrollees between 200 and 600 percent of the federal poverty level [i] including $349 million GF. In this allocation, 17 percent is for premium assistance for beneficiaries between 200 and 400 percent FPL and 83 percent for premium assistance for beneficiaries at or below 138 percent FPL and between 400 and 600 percent [ix]
- Support for Individuals Experiencing Homelessness: Allocates $550 million of the federal Coronavirus Relief Fund received by the state to Homekey, the state’s effort to secure hotels, motels, residential care facilities, and other housing for people experiencing homelessness and at risk of COVID-19. Additionally, $50 million GF is also included in the budget to acquire Homekey operating sites and provide initial operating subsidies. Homekey builds off Project Roomkey, which was a short-term emergency solution created in the early stages of the COVID-19 outbreak in California.
- EITC Tax Credit: The Budget maintains the Earned Income Tax Credit’s (EITC) extended level of credit included in the 2019 Budget Act, which offered tax credits to one million additional households. This includes $1,000 for every eligible family that also has at least one child under age six. [iii]
4. Safety Net Hospital, Clinic, and Provider Impacts
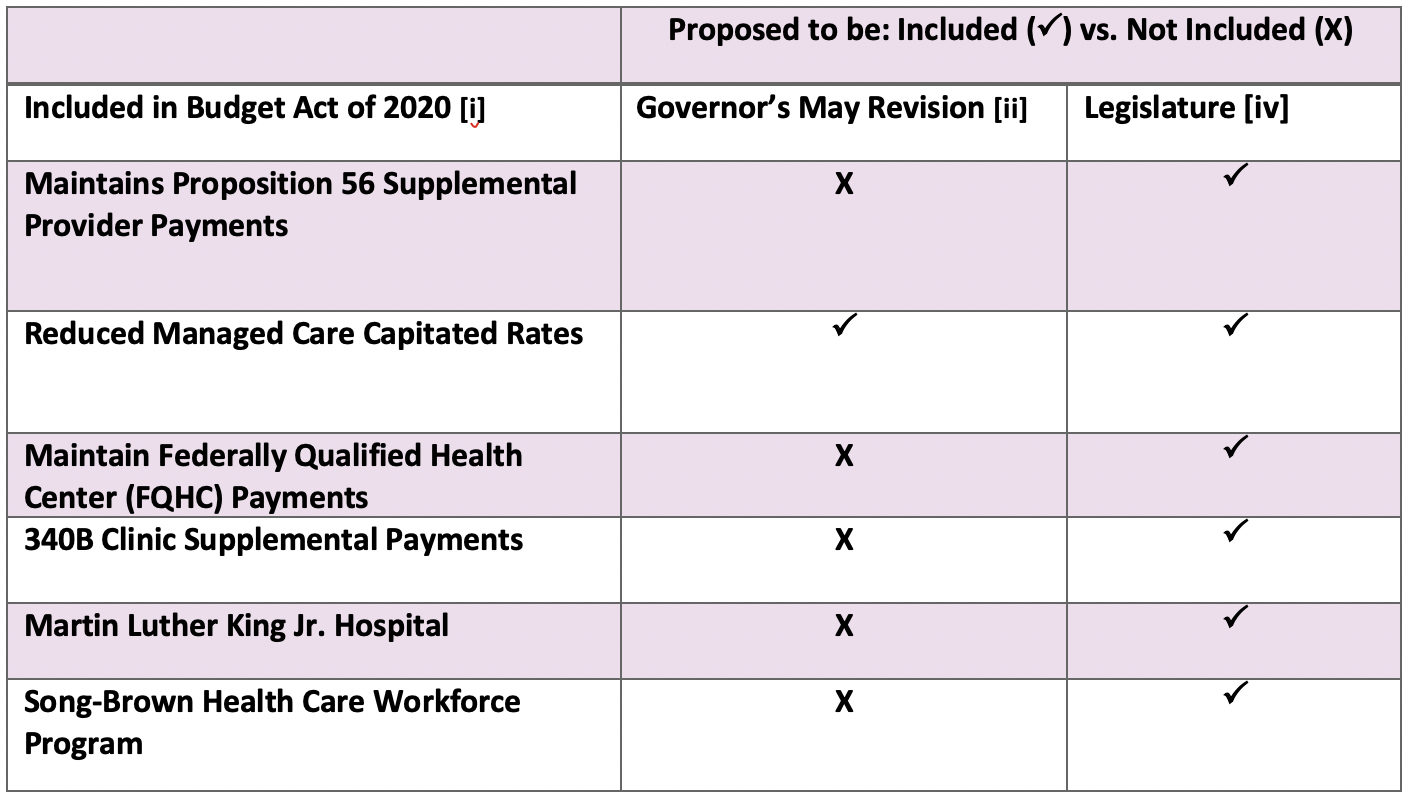
- Modifications to Proposition 56 Funding: Allocates $1.1 billion in Proposition 56 funding for supplemental payments, rate increases, and value-based payments. The 2020 – 2021 Budget Act maintains funding for the Physicians and Dentists Loan Repayment Programs. The Administration may suspend funding, starting July 1, 2020, for all programs except Loan Repayment Programs, women’s health, and family planning. The suspension may be lifted in next year’s budget. [i]
- Changes to Medi-Cal Managed Care Capitation Rates: Effective January 1, 2021, adjustments will be made to yield savings of $193.6 million ($63 million GF). [i]
- 340B Clinic Supplemental Payments: Allocates $52.5 million ($92.8 million GF) in FY 2020 – 2021 to provide supplemental payments to specific non-hospital clinics who participated in the federal 340B pharmacy program. These payments will grow to $105 million ($52.5 million GF) in FY 2021 – 2022. [i]
- Martin Luther King Jr. Hospital: Maintains supplemental payment to this hospital totaling $8.2 million GF. [i]
- Song-Brown Health Care Workforce Program: Maintains $33.3 million GF support for this health care workforce investment. [i]
5. Projected COVID-19 Costs Covered by Medi-Cal for the Uninsured and Underinsured
Since the May Revision and the onset of the COVID-19 crisis, DHCS requested federal approval for COVID-19-specific Medi-Cal program modifications through Section 1135 and 1115 waivers and State Plan Amendments; several of the federally approved modifications are listed below and are in place until the cessation of the COVID-19 crisis. [x]
- Uninsured Coverage Expansion: Provides coverage for diagnostic testing, treatment, and other COVID-19-related services to people who are uninsured, at no cost to them. These services are reimbursed at 100 percent federal funding.
- Hospital Presumptive Eligibility (HPE) Expansion: Expansion of HPE to include the aged (65 years of age and older), disabled, and blind population, including HPE coverage for two periods within a 12-month timeframe.
- Telehealth Services Flexibilities: Waives the face-to-face requirement for Medi-Cal beneficiaries, including for FQHCs and Rural Health Centers (RHCs) to allow health care services to be administered using all forms of telehealth or telephone platforms, regardless of a beneficiary’s location. This modification also authorizes payments that are not otherwise paid under Medi-Cal, including for FQHC/RHC, during the pandemic crisis.
[i] Office of the Governor, Enacted Budget Summary, June 2020.
[ii] Department of Health Care Services, 2020-21 May Revision Highlights, May 14, 2020.
[iii] Department of Finance, May Revision, Health and Human Services Budget Summary.
[iv] California State Assembly, Floor Report 2020-2021 State Budget, June 12, 2020.
[v] Public Health Omnibus, Chapter 12, Statutes of 2020, June 29, 2020.
[vi] Office of the Governor, Enacted Budget Summary for the Budget Act of 2019, June 2019.
[vii] California Department of Public Health, Black Infant Health, Program Profile, April 1, 2020.
[viii] Department of Aging, CBAS Center Overview, February 2020.
[x] Budget Act of 2020: Senate Bill (SB) 74, Chapter 6, Statutes of 2020.
[ix] Department of Health Care Services, State Plan Amendments approval letter DHCS 20-0024, May 2020.