Covered California Anticipates 500,000 – 1.2 Million More Uninsured Californians in 2019
In 2019, Covered California projects recent federal policy actions will drive up premiums, reduce enrollment, and increase the number of uninsured.
Last week Covered California announced its 2018-19 proposed budget, including estimated premium increases of between 9 and 13 percent for 2019. Similarly, states using the federal marketplace recently announced dramatic premium increases of up to 30 percent in the upcoming year. Across the board, these estimates reflect the negative impact of federal policy changes on enrollment and premiums in Covered California, and nationwide.
Impact of Eliminating the Individual Mandate Tax Penalty on Enrollment and Premiums
Multiple analyses project the elimination of the individual mandate tax penalty will decrease marketplace enrollment. Under the Affordable Care Act (ACA), individuals are mandated to have minimum coverage or pay a tax penalty (unless certain exemption criteria are met). The U.S. Senate tax bill (House Resolution 1, the Tax Cuts and Jobs Act) eliminates the financial penalty in 2019.
The individual mandate tax penalty incentivizes individuals that might not otherwise be compelled to pay for adequate coverage, such as young and/or healthy individuals. All individual market consumers are part of the same risk pool (financial risk for health coverage is shared by all consumers); and therefore, maximizing enrollment of young and healthy individuals helps keep premiums stable for the entire market.
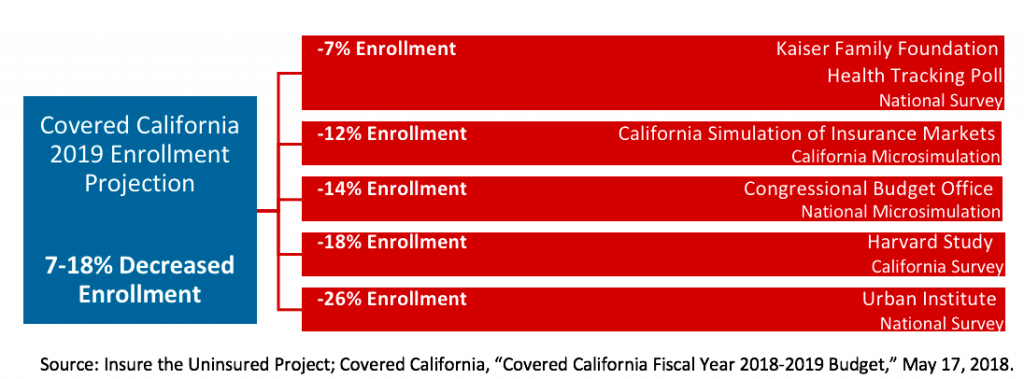
Without the individual mandate tax penalty, analyses project individual market enrollment will decrease nationally 7-26 percent in 2019.[1] In California, enrollment is expected to drop 7-18 percent in 2019, impacting between 152,000-393,000 Californians.[2] Declining enrollment will be concentrated among those previously motivated to secure coverage because of the individual mandate penalty, which tend to be young and healthy consumers. The following figure summarizes the analyses factored into Covered California’s enrollment projections.
Enrollment projections inform estimates on premiums including changes directly attributable to the elimination of the individual mandate tax penalty. Covered California projects a base 2019 premium increase of 11 percent, with the elimination of the individual mandate penalty responsible for 6 percent of the increase and the remainder primarily associated with health care cost trends.[3] (The base projection reflects the midpoint of the most optimistic and most pessimistic estimates.) Increases in premiums will likely lead to more individuals leaving the individual market, especially individuals who do not receive subsidies to offset increasing premium costs.
Covered California Efforts to Mitigate the Harm of Some Federal Policy Changes
In its role as an active purchaser, Covered California has taken steps to mitigate the harm of some federal policy changes that have adversely impacted other state exchanges and the federal marketplace.
Marketing and Outreach Spending. The federal government significantly reduced marketing and outreach funding for the 2018 annual open enrollment period. In anticipation of reduced federal funds for the 2018 open enrollment, Covered California augmented its marketing and outreach budget by $100 million. At the end of the 2018 open enrollment, Covered California enrollment remained stable while enrollment in the federal exchange declined.
For 2019, there is no indication that the federal government will reinstate funding for marketing and outreach; and therefore, similar efforts to augment Covered California’s marketing and outreach budget are already underway.
Elimination of Federal Funding for ACA Cost Sharing Reduction (CSR) Subsidies. In 2017, the Trump Administration ended federal funding to reimburse plans for providing CSR subsidies. The ACA requires insurers to reduce consumer cost sharing for those eligible and enrolled in a silver tier product, even if insurers are not reimbursed by the federal government.
Covered California developed a “work around” to address the elimination of federal funding for CSRs. Covered California worked with health plans to add a surcharge to marketplace silver tier products only to recoup the costs of CSR subsidies. Individuals eligible for ACA premium tax credits (consumers under 400 percent of the federal poverty level [FPL]) were protected from the increased costs of the surcharge because tax credits adjusted to cover the costs. Alternative products were developed outside the exchange for unsubsidized individuals interested in purchasing a silver tier plan and avoiding the surcharge.
For those unsubsidized consumers over 400 percent FPL, the federal decision to eliminate CSR subsidies significantly impacted premiums in silver tier exchange products and will likely continue to do so in 2019. The alternative products developed outside the exchange will also likely continue to mitigate the impact of this premium increase for unsubsidized consumers interested in enrolling in silver tier coverage.
California Policies to Strengthen the Individual Market
Without state or federal intervention, Covered California anticipates continued reductions in enrollment, increases in premiums, and growth in the rate of uninsured Californians beyond 2019.
Federal intervention to stabilize the individual market is unlikely, as outlined in the ITUP Blog, “Stabilizing the Individual Market after Federal Efforts Stall.” California lawmakers have taken some actions intended to stabilize enrollment, including ensuring Covered California consumers have an extended open enrollment period compared to the federal exchange shortened six-week period.
The March 2018 ITUP Blog outlines additional state market stabilization policies being considered in California including:
- State Funded Reinsurance or Invisible High-Risk Pool,
- State Mandate to Maintain Coverage,
- Protecting ACA Market Rules Against Federal Policy Changes, and
- State Subsidies to Address Affordability in the Individual Market.
Addressing the destabilizing impact of federal changes on California’s individual market falls to state lawmakers. California lawmakers have already introduced multiple bills to preserve the ACA market and stabilize the marketplace. (See ITUP blog on 2018 bills here.)
Without State Action the Uninsured Rate in California will Grow
In 2019, some Californians will choose to drop coverage because they no longer face a tax penalty. This exodus will cause premiums to rise, making coverage unaffordable for other Californians forced to drop coverage. According to an analysis prepared by PwC for the Covered California Board, between 500,000 and 1.2 million Californians will join the ranks of the uninsured in 2019 unless state lawmakers act to address the impact of federal policy changes.[4] Action this year to mitigate these affects will be important to protect the gains California made in reducing the number of uninsured.
[1] Covered California, “Covered California Fiscal Year 2018-2019 Budget,” May 17, 2018.
[2] Covered California, “Covered California Fiscal Year 2018-2019 Budget.”
[3] PwC, “Impact of Individual Mandate Penalty Elimination and Other Market Factors on Coverage Nationally and in California,” prepared for the Covered California Board, May 17, 2018.
[4] PwC, “Impact of Individual Mandate Penalty Elimination and Other Market Factors on Coverage Nationally and in California.”